October 21, 2020
2 min read

The percentage of adult arthritis visits to office-based physicians increased significantly during 2006-2015, with the percentage of visits where opioids were prescribed also increasing during that time, according to data.

Chad Helmick
“The 2016 CDC Guideline for Prescribing Opioids for Chronic Pain recommends nonpharmacologic therapy and nonopioid therapy for chronic pain, and consideration of opioid therapy for chronic pain-related conditions, including osteoarthritis, only if expected benefits for pain and function are anticipated to outweigh risk due to the possible harms of opioids,” Chad Helmick, MD, of the CDC’s National Center for Chronic Disease Prevention and Health Promotion, and leader of the CDC’s Arthritis Program, and colleagues wrote in Arthritis Care & Research.

The percentage of adult arthritis visits to office-based physicians increased significantly during 2006-2015, with the percentage of visits were opioids were prescribed also increasing during that time, according to data
“Moreover, opioids to treat moderate to severe chronic back, hip or knee osteoarthritis pain have not been superior to nonopioid medications,” they added. “There are gaps in literature regarding the use of prescription opioids for adults with arthritis in the ambulatory care setting, where most arthritis is diagnosed and managed.”
To examine U.S. opioid prescription trends during adult office visits for arthritis from 2006 to 2015, Helmick and colleagues analyzed data from the National Ambulatory Medical Care Survey (NAMCS). According to the researchers, NAMCS is an annual, nationally representative survey of visits to nonfederal, office-based physicians in the United States, conducted by the National Center for Health Statistics.
The researchers analyzed visit percentages for first- and any-listed arthritis by age and sex. Arthritis was defined using the ICD-9-CM codes 274, 710, 712-716, 719, 729.1, based on a subset of arthritis codes originally described by the National Arthritis Data Workgroup. In addition, Santo and colleagues grouped time periods into 2-year intervals, which they said increased the reliability of their estimates. Lastly, they used linear regression models to report annual percentage changes and confidence intervals.
According to the researchers, the percentage of visits to officebased physicians by adults with a firstlisted arthritis diagnoses increased from 4.1% (95% CI, 3.5% to 4.7%) in 20062007, to 5.1% (95% CI, 3.9% to 6.6%) in 20142015 (P = .033). Meanwhile, the percentage of these visits in which opioids were prescribed increased from 16.5% (95% CI, 13.1% to 20.5%) in 20062007, to 25.6% (95% CI, 17.9% to 34.6%) in 20142015 (P = .017).
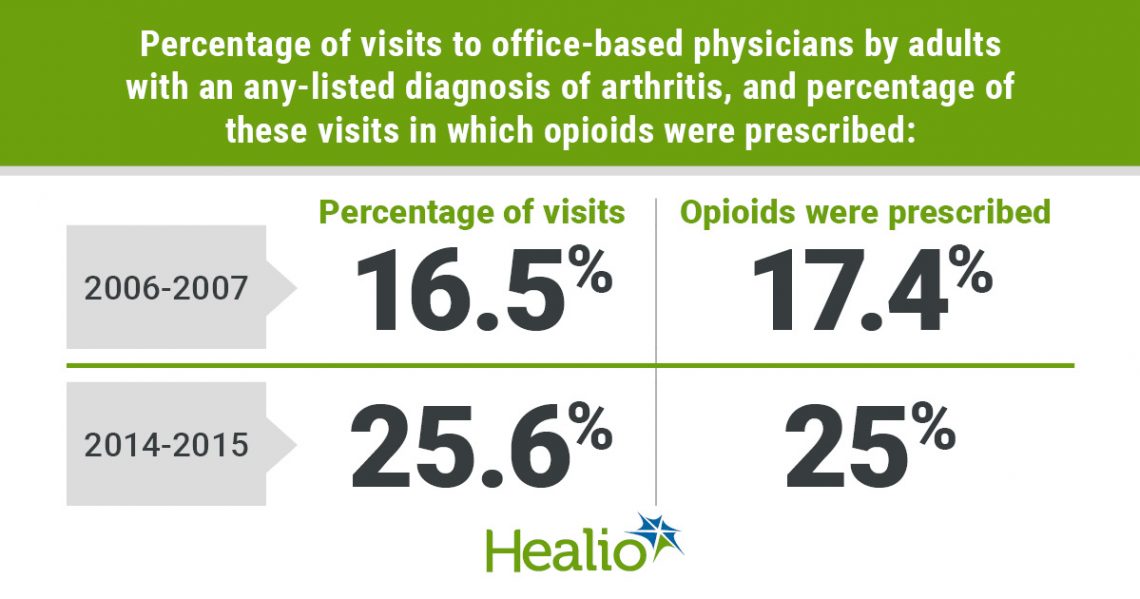
For office visits with any-listed diagnoses of arthritis, the percentage increased from 16.5% (95% CI, 13.1% to 20.5%) in 20062007, to 25.6% (95% CI, 17.9% to 34.6%) in 20142015 (P = .017). Among these visits, the percentage in which opioids were prescribed increased from 17.4% (95% CI, 14.6% to 20.4%) in 20062007, to 25% (95% CI, 19.7% to 30.8%) in 20142015 (P = .004).
“The office visits for arthritis increased from 2006 through 2015 and the proportion of those visits with opioids prescribed increased as well,” Helmick told Healio Rheumatology. “This may have been because of the general increase during this period in opioid use for managing chronic pain. Better surveillance of chronic pain, especially among the large population with arthritis and chronic pain, is needed to monitor how the opioid crisis is changing pain management — for better or worse.”
“More opioid prescriptions during this time period for this common condition, along with a report that those with arthritis comprise the majority of those prescribed opioids, indicate that the growing ambulatory care problem of arthritis pain management will likely increase,” he added. “Better non-opioid pain management may help reduce this problem and help with the opioid crisis as well.”