Subjective cognitive decline (SCD) is a person’s perception of their worsening cognitive functions or more frequent confusion or memory loss in the past 12 months and is an early symptom of Alzheimer’s disease (Taylor et al., 2018; Wang et al., 2018). Usually, there is normal performance on standardized tests for cognition (Studart & Nitrini, 2016). According to Taylor et al. (2018), approximately 11% of adults age ≥45 years in the United States report SCD. In addition, one half of these adults report associated functional limitations (Taylor et al., 2018). SCD has also been found to be positively associated with depression (Zlatar, Muniz, Galasko, & Salmon, 2018; Zlatar, Muniz, Espinoza, et al., 2018); poorer overall (Tales et al., 2015) and health-related (Roehr et al., 2017) quality of life; increased risk of mortality (Luck et al., 2015); and significant public health and economic impact (Lin & Neumann, 2013).
Sociodemographic characteristics, health outcomes, and behaviors are associated with SCD. SCD is also more common among older adults (Taylor et al., 2018; Zlatar, Muniz, Galasko, & Salmon, 2018). Racial/ethnic differences also exist in SCD, where it is more commonly reported among Black, American Indian/Alaska Natives, and Other/Multiracial adults compared to other racial/ethnic groups (Taylor et al., 2018). Adults with lower educational attainment and those who are unemployed also report more SCD compared to adults with higher educational attainment and employment, respectively (Taylor et al., 2018). Diabetes (Andersen et al., 2019; Ng et al., 2016; Yin et al., 2016; Zhang et al., 2019), obesity (Noh et al., 2019; Olivo et al., 2019), and smoking (Anstey et al., 2007; Depp et al., 2015; Hu et al., 2019; Mucha et al., 2006) were found to be positively associated with cognitive impairment. SCD has also been positively associated with depression (Wei et al., 2019; Zlatar, Muniz, Galasko, & Salmon, 2018; Zlatar, Muniz, Espinoza, et al., 2018) and anxiety (Tandetnik et al., 2017) among older adults.
Informal caregiving continues to be an integral component of society, the health care system, and economy of the United States (Schulz & Tompkins, 2010). An informal caregiver is defined as a person who provides care (assistance with activities of daily living [ADLs] or instrumental ADLs [IADLs]), usually unpaid, to family or friends (Roth et al., 2015; Schulz & Tompkins, 2010). Greater informal caregiving may be associated with health benefits among caregivers (Kim et al., 2019; Roth et al., 2015). Nevertheless, being an informal caregiver can be demanding and may also have detrimental effects on the caregiver’s health and well-being, usually referred to as caregiver burden. Caregiver burden has been linked to reduced life satisfaction (Hajek & König, 2018), psychological distress (Abreu et al., 2018), poorer self-reported health status (Do et al., 2014), and lower quality of life (Alltag et al., 2018; Lethin et al., 2018). Most informal caregivers are themselves either older or middle-aged adults, many of whom must balance competing family and employment obligations (Ryan et al., 2012).
Informal caregiving and SCD are linked to physical health and health behaviors. One study found that 82% of caregivers reported at least one chronic condition (Wang et al., 2014), and multiple chronic conditions may lead to adverse emotional and physical health outcomes among caregivers (Polenick et al., 2020). SCD has also been found to be statistically significantly associated with heart disease, stroke, and multimorbidity (Yap et al., 2020). Previous research using a nationally representative sample found that 15% of respondents with at least one chronic illness reported SCD (Taylor et al., 2018). Another study also showed that caregiving was positively associated with diabetes (Stacey et al., 2018). Health behaviors, including smoking (Dich et al., 2016; Hopps et al., 2017; Stacey et al., 2018), alcohol use (Dich et al., 2016; Kearns et al., 2017), and physical activity (Cuthbert et al., 2017) are associated with caregiving and may act as potential covariates in the relationship between caregiving and SCD.
Informal caregiving has also been linked to better (Bertrand et al., 2012) and worse (Mallya & Fiocco, 2018) objective cognition. Among female caregivers, caregiving was associated with better cognitive function compared to non-caregivers (Bertrand et al., 2012; Zwar et al., 2018), but there was no association among male caregivers (Zwar et al., 2018). The association between informal caregiving and better objective cognitive functioning has also been found among White populations but not among Black populations (Sneed et al., 2019). Among a Canadian population, caregivers were found to experience lower objective cognition, more perceived stress, lower quality of life, and depressive symptoms (Mallya & Fiocco, 2018). Based on these findings, it is possible that informal caregiving may be associated with SCD. However, to our knowledge, no study has examined the association between informal caregiving and SCD among a population-based sample. In addition, studies examining gender differences in the relationships between informal caregiving, poor mental health, and SCD among population-based samples are lacking. It is also possible that if there are relationships between SCD and informal caregiving, they may differ for men and women.
One conceptual framework that may help in understanding the association between informal caregiving, poor mental health, and SCD among caregivers is the theoretical model of stress and health/illness (Vitaliano et al., 2003). This model states that exposure to stress among caregivers may lead to psychological distress and impact health behaviors, which are associated with physiological responses, which increase the likelihood of illness. Informal caregiving may represent exposure to stress, poor mental health as psychological distress, and the related physiological responses may result in or exacerbate existing SCD. Evidence of this model exists in the literature where informal caregiving is associated with cognitive impairment (Brummett et al., 2013; Mallya & Fiocco, 2018) among caregivers. Another aspect of this framework considers gender as a moderator. Gender refers to the cultural aspects and roles that distinguish female and male caregivers (Muehlenhard & Peterson, 2011). Findings showed that female caregivers reported worse global health compared to male caregivers (Vitaliano et al., 2003). However, to our knowledge, no study has examined the gender differences in the relationship between informal caregiving and SCD.
Caregiver burden has been found to be associated with SCD but this association has been examined by assessing burden among caregivers and SCD among their caregiving recipients (Dauphinot et al., 2016). Studies examining the relationship between caregiving and SCD among caregivers are lacking. In addition, research assessing the gender differences in the role of poor mental health in SCD and informal caregiving is also sparse. Using the theoretical model of stress and health/illness, it is possible that informal caregiving may be linked to poor mental health, which may impact SCD, and that gender may play a role. Therefore, the aims of the current study were to: (a) determine the association between informal caregiving and poor mental health; (b) assess the association between poor mental health and SCD; (c) explore the association between informal caregiving and SCD; and (d) assess the moderation of these potential associations by gender. We hypothesized that: (H1) informal caregiving would be associated with poor mental health; (H2) poor mental health would be linked to greater SCD; (H3) informal caregiving would be positively associated with SCD; and (H4) differences would be observed for men and women in the relationship between caregiving and SCD, where women would have a stronger association between informal caregiving and SCD. By examining the gender differences in poor mental health, caregiving, and SCD, these findings will help inform population-based interventions aimed at improving SCD and poor mental health of informal caregivers and inform clinicians if gender differences should be considered in approaches to clinical care.
Method
Data Source and Study Population
This cross-sectional study used data from the 2016 Behavioral Risk Factor Surveillance System (BRFSS) (Centers for Disease Control and Prevention [CDC], 2018). Established by the CDC, the BRFSS is a set of health-related surveys administered to residents in the United States. The cognitive decline module was only asked of participants aged ≥45 years. There were 18,357 respondents aged ≥45 in Montana, New Jersey, Oregon, and Tennessee. Respondents who were missing or did not give valid answers on the caregiver and cognitive decline questions were excluded (n = 2,310). The University of South Carolina Institutional Review Board considered the current study “not human subjects research” as deidentified publicly available data were used.
Measures
The question that operationalized caregiving stated: “During the past 30 days, did you provide regular care or assistance to a friend or family member who has a health problem or disability?” This question also measures physical dependence of the caregiving recipient (Perenboom & Chorus, 2003). Poor mental health was operationalized by the question: “Now thinking about your mental health, which includes stress, depression, and problems with emotions, for how many days during the past 30 days was your mental health not good?” This question measures a key component of the CDC’s health-related quality of life concept (CDC-HRQOL) (Yin et al., 2016). The question that operationalized SCD was only asked of respondents aged ≥45 years: “During the past 12 months, have you experienced confusion or memory loss that is happening more often or is getting worse?” This question has been used to operationalize SCD in previous studies (Anderson et al., 2015; Taylor et al., 2018). The total number of respondents who answered “yes” or “no” to both the caregiver and cognitive decline modules, and whose reported gender was known, was 16,042 (n = 9,410 women; n = 6,632 men).
Covariates
Sociodemographic characteristics considered as covariates were age (60 to 69 [young-old], 70 to 79 [middle-old], 80+ [old-old] [Forman et al., 1992] vs. 45 to 59 [middle-aged]); annual household income (<$15,000, $15,000 to <$50,000 vs. $50,000+); educational attainment (less than high school, high school graduate, greater than high school); employment (employed, retired vs. unemployed); and race/ethnicity (Black, non-Hispanic; Other, non-Hispanic; and Hispanic vs. White, non-Hispanic). Additional variables considered as covariates included diabetes (yes vs. no [including only during pregnancy]); obesity (body mass index [BMI] ≥30 kg/m2 vs. <30 kg/m2); current smoking (now smokes every day or some days vs. former smoker/never smoked); alcohol use (number of drinks per day when drinking), and physical activity (e.g., running, calisthenics, golf, gardening, walking) in the past 30 days (yes vs. no). We considered heart disease but several studies found that the risk of heart disease was similar between caregivers and non-caregivers (Buyck et al., 2013; Haley et al., 2010; Liu & McDaniel, 2015; Miyawaki et al., 2017). Therefore, heart disease was not included in the fully adjusted model.
Data Analysis
All analyses considered the BRFSS complex multistage sampling strategy. Weighted prevalence estimates were obtained for informal caregiving and SCD, overall and by sociodemographic characteristics. Chi-square p values were used to compare the distributions of gender, age, income, education, employment, race/ethnicity, heart disease, diabetes, obesity, current smoking, and physical activity by caregiving and SCD status. The distribution of caregiving characteristics was also obtained overall, and among men and women. Covariates that were considered were based on a priori literature review, were associated with caregiving, and were independent risk factors for SCD.
Simple and multiple linear regression models were used to determine the crude and adjusted βs and 95% confidence intervals (CIs) depicting the associations between informal caregiving and poor mental health. Crude and multivariate logistic regression models were also used to determine crude and adjusted odds ratios (ORs) and 95% CIs for the association between poor mental health and SCD, and between caregiving and SCD. Model 1 was the unadjusted or crude model. Model 2 was the fully adjusted model, which controlled for all sociodemographic and health characteristics: age, income, educational attainment, work, race/ethnicity, diabetes, obesity, current smoking, alcohol use, and physical activity. Based on prior research, where a higher percentage of caregivers are women (National Alliance for Caregiving & AARP Public Policy Institute, 2015), models were stratified by gender.
All analyses considered the complex multistage sampling design by using weighted data using sample weights provided in the BRFSS sample and were conducted with SAS software version 9.4.
Results
Overall, 24% of respondents reported being caregivers in the past 30 days and 11% of respondents reported SCD. Approximately 21% of men and 26% of women reported being caregivers in the past 30 days. However, 11% of both men and women reported SCD. The overall mean number of days of poor mental health in the past 1 month was 12.3 (SD = 0.28 days), 12.4 (SD = 0.48 days), and 12.3 (SD = 0.33 days) for men and women, respectively.
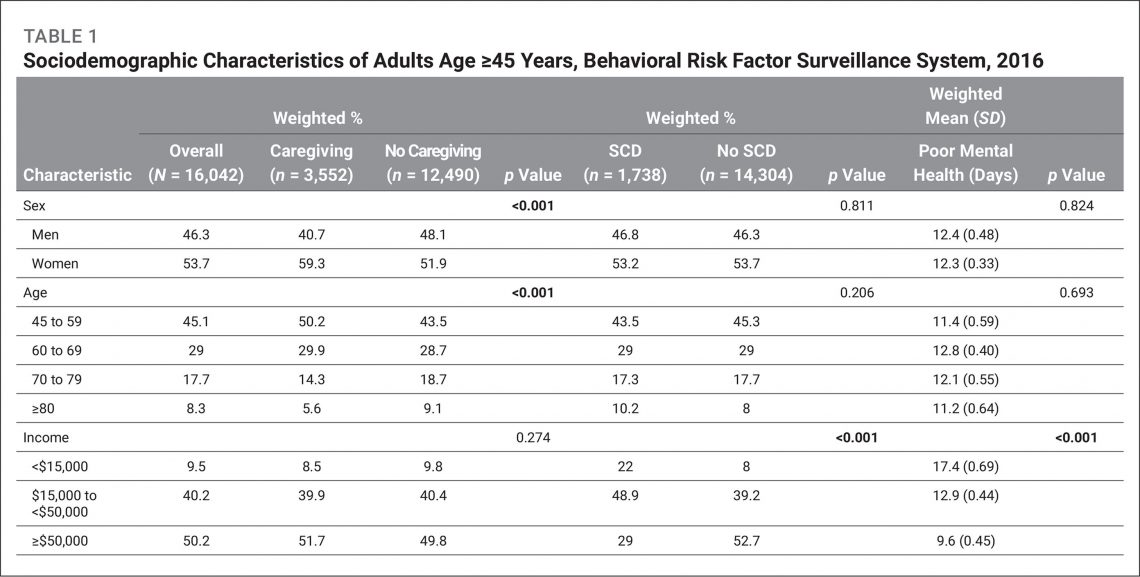
Table 1 shows the sociodemographic characteristics, physical health, and risk behaviors of respondents aged ≥45 years and the distribution of reported caregiving, SCD, and poor mental health. There were statistically significant differences by gender, age, educational attainment, employment, race/ethnicity, obesity, and current smoking status in caregiving (p < 0.05). The difference in informal caregiving by physical activity status was not statistically significant (p = 0.058). Respondents who reported caregiving tended to be women, younger (age 45 to 59), have higher educational attainment, employed or unemployed (not retired), White, BMI ≥30 kg/m2, and current smokers. There were also statistically significant differences by annual household income, educational attainment, employment, race/ethnicity, heart disease, diabetes, obesity, current smoking, and physical activity in SCD (p < 0.05). Respondents who reported SCD tended to report an annual household income of <$50,000 per year, lower educational attainment, unemployment, were of “Other, non-Hispanic” race or Hispanic ethnicity, and reported heart disease, diabetes, obesity, current smoking, and no physical activity. Statistically significant differences existed in poor mental health by income, education, employment, heart disease, diabetes, obesity, current smoking, alcohol use, and physical activity (p < 0.05).
   |
Table 1: Sociodemographic Characteristics of Adults Age ≥45 Years, Behavioral Risk Factor Surveillance System, 2016 |
Table 2 shows the distribution of caregiving characteristics overall and among men and women. Statistically significant differences by gender existed in relationship to caregiving recipient and time spent caregiving. For example, a higher percent of women compared to men cared for a parent (33.6% vs. 27.3%), whereas a higher percent of men cared for their spouse or partner (22.4% vs. 16.7%). Women also tended to report more caregiving hours per week compared to men (≥40 hours: 23.7% vs. 18.5%).
 |
Table 2: Caregiving Characteristics Overall and Among Men and Women |
Table 3 shows the overall association between informal caregiving, poor mental health, and SCD among respondents age ≥45 years for the overall sample, and among men and women. After adjusting for sociodemographic characteristics, physical health, and health behaviors, respondents who reported informal caregiving reported 1 additional day of poor mental health per month (adjusted β = 1.26; 95% CI [0.87, 1.64]). In addition, a 1-day increase in poor mental health in the past 1 month was associated with a 5% increase in the odds of reporting SCD (adjusted OR = 1.05; 95% CI [1.03, 1.07]). After adjustment for covariates, the association between caregiving and SCD was not statistically significant.
After adjusting for sociodemographic characteristics, physical health, and health behaviors in the fully adjusted model, men who reported informal caregiving reported approximately 3 additional days of poor mental health in the past 1 month (adjusted β = 2.60; 95% CI [2.59, 2.62]). A 1-day increase in poor mental health in the past 1 month was associated with a 5% increase in the odds of reporting SCD (adjusted OR = 1.05; 95% CI [1.02, 1.08]). In addition, men who reported informal caregiving had statistically similar odds of reporting SCD when compared to men who did not report informal caregiving (adjusted OR = 1.56; 95% CI [0.93, 2.63]). Fully adjusted models also showed that women who reported caregiving reported more time of poor mental health in the past 1 month compared to women who did not report informal caregiving (adjusted β = 0.40; 95% CI [0.23, 0.57]). A 1-day increase in poor mental health in the past 1 month was associated with a 7% increase in the odds of reporting SCD (adjusted OR = 1.07; 95% CI [1.04, 1.10]). However, the association between caregiving and SCD was not statistically significant among women (adjusted OR = 1.34; 95% CI [0.74, 2.42]).
Discussion
To our knowledge, this is the first study examining the association among informal caregiving, poor mental health, and SCD in U.S. adult caregivers. The main findings of the current study were that informal caregiving was positively associated with poor mental health, and poor mental health was positively associated with SCD among men and women. This study is among the first to show that the association between informal caregiving and SCD was not statistically significant among men or women.
The conceptual framework by Vitaliano et al. (2003) suggests that exposure to stress among caregivers may lead to psychological distress and increased illness, and female caregivers tend to report worse global health compared to male caregivers. Our results partially supported this model. Informal caregiving was associated with poor mental health and a stronger association was seen among men compared to women. This finding supports previous research, which shows that a higher proportion of male caregivers report greater mental health symptoms, such as anxiety or depressive symptoms, compared to their female counterparts (Oechsle et al., 2013). However, the relationship between informal caregiving and SCD was not statistically significant in this population. Another study among a German population found that looking after someone was associated with better cognitive functioning among women but there was no statistically significant association in men (Zwar et al., 2018), which partially supports our results as the association between informal caregiving and SCD was not statistically significant among women or men. Different populations and varying cultural expectations may have played a role in these disparate findings.
Poor mental health was associated with SCD among men and women in the current study. Psychological distress was associated with subjective cognitive complaints among patients with brain tumor (Pranckeviciene et al., 2017) and a potential reciprocal relationship has been found between depression and subjective cognitive impairment (Hill et al., 2016), which supports the current study’s findings. A relationship has also been found between SCD and anxiety, which seems to be driven by concerns about functional impairment (Hill et al., 2016).
Limitations and Strengths
There are some limitations to consider in the context of these findings. The study was cross-sectional. Respondents were asked about their informal caregiving responsibilities in the past 30 days and about their SCD in the past 12 months. Therefore, it is possible that SCD may have occurred before informal caregiving. As a result, causation cannot be inferred. Therefore, these results highlight the need for longitudinal studies determining the relationship between these key variables. Data were also self-reported, which may result in overreporting or underreporting of key variables, such as informal caregiving or SCD. These alterations may result in underestimates or overestimates of the “true” association. The study sample was a population-based sample from four states in the United States (Montana, New Jersey, Oregon, and Tennessee), and may not be generalizable to other states or countries. Only a few questions were used to quantify informal caregiving and poor mental health. Indeed, the definition of caregiver in the BRFSS does not require the caregiver to provide ADL or IADL tasks, which are key components of caregiving. We were unable to include number of care hours and caregiving recipient in the model due to high correlations and these variables being a subset of the caregiving (exposure) variable due to skip patterns in the survey. Lastly, as it was only possible to control for several well-established confounding variables, such as age, income, education, employment, race/ethnicity, chronic illnesses, and health behaviors, there may be residual confounding due to unmeasured variables (e.g., hypertension) not used as covariates in this analysis.
Nevertheless, the study had notable strengths. The study sample size was large (N = 16,042) and population-based. All analyses also considered the BRFSS complex multistage sampling strategy. Adjusted analyses controlled for sociodemographic covariates, which may alter the association between informal caregiving and SCD. In addition, findings were stratified by gender. This strategy is crucial in helping inform the importance of the consideration of gender differences in examining informal caregiving, poor mental health, and SCD, which may have potential importance in the development of theory-based interventions and programs designed to reduce caregiver burden and improve caregiver quality of life among middle-aged and older adults.
Conclusion
The association between informal caregiving and SCD was not statistically significant, although stronger for men than women. Informal caregiving was associated with poor mental health among men and women, with a stronger association among men. Poor mental health was associated with SCD with similar associations among men and women. Additional studies are needed that will identify key variables influencing SCD among male and female informal caregivers. The findings also warrant longitudinal mediation studies where the temporal sequence among caregiving, poor mental health, and SCD may be established to determine target populations and focal points of intervention and prevention programs. Qualitative studies may also assess potential reasons for the apparent differences in the relationship between informal caregiving and poor mental health among men and women.
References
- Abreu, W., Tolson, D., Jackson, G. A. & Costa, N. (2020). A cross-sectional study of family caregiver burden and psychological distress linked to frailty and functional dependency of a relative with advanced dementia. Dementia (London), 19(2), 301–318 doi:10.1177/1471301218773842 [CrossRef] PMID:29717622
- Alltag, S., Conrad, I. & Riedel-Heller, S. G. (2019). Caregiver burden among older informal caregivers of patients with dementia and its influence on quality of life: A systematic literature review [article in German]. Zeitschrift für Gerontologie und Geriatrie, 52, 477–486 doi:10.1007/s00391-018-1424-6 [CrossRef] PMID:29992357
- Andersen, S. L., Sweigart, B., Sebastiani, P., Drury, J., Sidlowski, S. & Perls, T. T. (2019). Reduced prevalence and incidence of cognitive impairment among centenarian offspring. The Journals of Gerontology. Series A, Biological Sciences and Medical Sciences, 74, 108–113 doi:10.1093/gerona/gly141 [CrossRef] PMID:29931286
- Anderson, L. A., Deokar, A., Edwards, V. J., Bouldin, E. D. & Greenlund, K. J. (2015). Demographic and health status differences among people aged 45 or older with and without functional difficulties related to increased confusion or memory loss, 2011 Behavioral Risk Factor Surveillance System. Preventing Chronic Disease, 12, E30 doi:10.5888/pcd12.140429 [CrossRef] PMID:25742067
- Anstey, K. J., von Sanden, C., Salim, A. & O’Kearney, R. (2007). Smoking as a risk factor for dementia and cognitive decline: A meta-analysis of prospective studies. American Journal of Epidemiology, 166, 367–378 doi:10.1093/aje/kwm116 [CrossRef] PMID:17573335
- Bertrand, R. M., Saczynski, J. S., Mezzacappa, C., Hulse, M., Ensrud, K. & Fredman, L. (2012). Caregiving and cognitive function in older women: Evidence for the healthy caregiver hypothesis. Journal of Aging and Health, 24, 48–66 doi:10.1177/0898264311421367 [CrossRef] PMID:21934121
- Brummett, B. H., Austin, S. B., Welsh-Bohmer, K. A., Williams, R. B. & Siegler, I. C. (2013). Long-term impact of caregiving and metabolic syndrome with perceived decline in cognitive function 8 years later: A pilot study suggesting important avenues for future research. Open Journal of Medical Psychology, 2, 23–28 doi:10.4236/ojmp.2013.21005 [CrossRef] PMID:24634805
- Buyck, J. F., Ankri, J., Dugravot, A., Bonnaud, S., Nabi, H., Kivimäki, M. & Singh-Manoux, A. (2013). Informal caregiving and the risk for coronary heart disease: The Whitehall II study. The Journals of Gerontology. Series A, Biological Sciences and Medical Sciences, 68, 1316–1323 doi:10.1093/gerona/glt025 [CrossRef] PMID:23525476
- Centers for Disease Control and Prevention. (2018). Behavioral risk factor surveillance system. https://www.cdc.gov/brfss/index.html
- Cuthbert, C. A., King-Shier, K., Tapp, D., Ruether, D. & Culos-Reed, S. N. (2017). Exploring gender differences in self-reported physical activity and health among older caregivers. Oncology Nursing Forum, 44, 435–445 doi:10.1188/17.ONF.435-445 [CrossRef] PMID:28632242
- Dauphinot, V., Ravier, A., Novais, T., Delphin-Combe, F., Mouchoux, C. & Krolak-Salmon, P. (2016). Risk factors of caregiver burden evolution for patients with subjective cognitive decline or neurocognitive disorders: A longitudinal analysis. Journal of the American Medical Directors Association, 17, 1037–1043 doi:10.1016/j.jamda.2016.07.003 [CrossRef] PMID:27575984
- Depp, C. A., Bowie, C. R., Mausbach, B. T., Wolyniec, P., Thornquist, M. H., Luke, J. R., McGrath, J. A., Pulver, A. E., Patterson, T. L. & Harvey, P. D. (2015). Current smoking is associated with worse cognitive and adaptive functioning in serious mental illness. Acta Psychiatrica Scandinavica, 131, 333–341 doi:10.1111/acps.12380 [CrossRef] PMID:25559296
- Dich, N., Head, J. & Hulvej Rod, N. (2016). Role of psychosocial work factors in the relation between becoming a caregiver and changes in health behaviour: Results from the Whitehall II cohort study. Journal of Epidemiology and Community Health, 70, 1200–1206 doi:10.1136/jech-2015-206463 [CrossRef] PMID:27217534
- Do, E. K., Cohen, S. A. & Brown, M. J. (2014). Socioeconomic and demographic factors modify the association between informal caregiving and health in the Sandwich Generation. BMC Public Health, 14, 362 doi:10.1186/1471-2458-14-362 [CrossRef] PMID:24735495
- Forman, D. E., Berman, A. D., McCabe, C. H., Baim, D. S. & Wei, J. Y. (1992). PTCA in the elderly: The “young-old” versus the “old-old.”Journal of the American Geriatrics Society, 40, 19–22 doi:10.1111/j.1532-5415.1992.tb01823.x [CrossRef] PMID:1727842
- Hajek, A. & König, H. H. (2018). The relation between personality, informal caregiving, life satisfaction and health-related quality of life: Evidence of a longitudinal study. Quality of Life Research, 27, 1249–1256 doi:10.1007/s11136-018-1787-6 [CrossRef] PMID:29335851
- Haley, W. E., Roth, D. L., Howard, G. & Safford, M. M. (2010). Caregiving strain and estimated risk for stroke and coronary heart disease among spouse caregivers: Differential effects by race and sex. Stroke, 41, 331–336 doi:10.1161/STROKEAHA.109.568279 [CrossRef] PMID:20075357
- Hill, N. L., Mogle, J., Wion, R., Munoz, E., DePasquale, N., Yevchak, A. M. & Parisi, J. M. (2016). Subjective cognitive impairment and affective symptoms: A systematic review. The Gerontologist, 56, e109–e127 doi:10.1093/geront/gnw091 [CrossRef] PMID:27342440
- Hopps, M., Iadeluca, L., McDonald, M. & Makinson, G. T. (2017). The burden of family caregiving in the United States: Work productivity, health care resource utilization, and mental health among employed adults. Journal of Multidisciplinary Healthcare, 10, 437–444 doi:10.2147/JMDH.S135372 [CrossRef] PMID:29255364
- Hu, M., Yin, H., Shu, X., Jia, Y., Leng, M. & Chen, L. (2019). Multi-angles of smoking and mild cognitive impairment: Is the association mediated by sleep duration?Neurological Sciences, 40, 1019–1027 doi:10.1007/s10072-019-03750-5 [CrossRef] PMID:30778881
- Kearns, N. T., Blumenthal, H., Rainey, E. E., Bennett, M. M., Powers, M. B., Foreman, M. L. & Warren, A. M. (2017). Discrepancy in caregiving expectations predicts problematic alcohol use among caregivers of trauma injury patients six months after ICU admission. Psychology of Addictive Behaviors, 31, 497–505 doi:10.1037/adb0000282 [CrossRef] PMID:28493754
- Kim, G., Allen, R. S., Wang, S. Y., Park, S., Perkins, E. A. & Parmelee, P. (2019). The relation between multiple informal caregiving roles and subjective physical and mental health status among older adults: Do racial/ethnic differences exist?The Gerontologist, 59(3), 499–508 doi:10.1093/geront/gnx196 [CrossRef] PMID:29373738
- Lethin, C., Leino-Kilpi, H., Bleijlevens, M. H., Stephan, A., Martin, M. S., Nilsson, K., Nilsson, C., Zabalegui, A. & Karlsson, S. (2018). Predicting caregiver burden in informal caregivers caring for persons with dementia living at home: A follow-up cohort study. Dementia (London), 19(3), 640–660 doi:10.1177/1471301218782502 [CrossRef] PMID:29929383
- Lin, P. J. & Neumann, P. J. (2013). The economics of mild cognitive impairment. Alzheimer’s & Dementia, 9(1), 58–62 doi:10.1016/j.jalz.2012.05.2117 [CrossRef] PMID:23141385
- Liu, L. W. & McDaniel, S. A. (2015). Family caregiving for immigrant seniors living with heart disease and stroke: Chinese Canadian perspective. Health Care for Women International, 36(12), 1327–1345 doi:10.1080/07399332.2015.1038346 [CrossRef] PMID:25985230
- Luck, T., Roehr, S., Jessen, F., Villringer, A., Angermeyer, M. C. & Riedel-Heller, S. G. (2015). Mortality in individuals with subjective cognitive decline: Results of the Leipzig Longitudinal Study of the Aged (LEILA75+). Journal of Alzheimer’s Disease, 48(Suppl. 1), S33–S42 doi:10.3233/JAD-150090 [CrossRef] PMID:26402077
- Mallya, S. & Fiocco, A. J. (2018). Impact of informal caregiving on cognitive function and well-being in Canada. International Psychogeriatrics, 30, 1049–1055 doi:10.1017/S1041610217002605 [CrossRef] PMID:29235432
- Miyawaki, A., Tomio, J., Kobayashi, Y., Takahashi, H., Noguchi, H. & Tamiya, N. (2017). Impact of long-hours family caregiving on non-fatal coronary heart disease risk in middle-aged people: Results from a longitudinal nationwide survey in Japan. Geriatrics & Gerontology International, 17(11), 2109–2115 doi:10.1111/ggi.13061 [CrossRef] PMID:28464424
- Mucha, L., Stephenson, J., Morandi, N. & Dirani, R. (2006). Meta-analysis of disease risk associated with smoking, by gender and intensity of smoking. Gender Medicine, 3, 279–291 doi:10.1016/S1550-8579(06)80216-0 [CrossRef] PMID:17582369
- Muehlenhard, C. L. & Peterson, Z. D. (2011). Distinguishing between sex and gender: History, current conceptualizations, and implications. Sex Roles, 64(11–12), 791–803 doi:10.1007/s11199-011-9932-5 [CrossRef]
- National Alliance for Caregiving, & AARP Public Policy Institute. (2015). Caregiving in the US. https://www.aarp.org/content/dam/aarp/ppi/2015/caregiving-in-the-united-states-2015-report-revised.pdf
- Ng, T. P., Feng, L., Nyunt, M. S., Feng, L., Gao, Q., Lim, M. L., Collinson, S. L., Chong, M. S., Lim, W. S., Lee, T. S., Yap, P. & Yap, K. B. (2016). Metabolic syndrome and the risk of mild cognitive impairment and progression to dementia: Follow-up of the Singapore Longitudinal Ageing Study Cohort. JAMA Neurology, 73(4), 456–463 doi:10.1001/jamaneurol.2015.4899 [CrossRef] PMID:26926205
- Noh, H. M., Han, J., Kim, Y. J., Jung, J. H., Roh, Y. K. & Song, H. J. (2019). Sex differences in the relationship between cognitive impairment and overweight or obesity in late life: A 3-year prospective study. Medicine, 98, e14736 doi:10.1097/MD.0000000000014736 [CrossRef] PMID:30817627
- Oechsle, K., Goerth, K., Bokemeyer, C. & Mehnert, A. (2013). Anxiety and depression in caregivers of terminally ill cancer patients: Impact on their perspective of the patients’ symptom burden. Journal of Palliative Medicine, 16, 1095–1101 doi:10.1089/jpm.2013.0038 [CrossRef] PMID:23909373
- Olivo, G., Gour, S. & Schiöth, H. B. (2019). Low neuroticism and cognitive performance are differently associated to over-weight and obesity: A cross-sectional and longitudinal UK Biobank study. Psycho-neuroendocrinology, 101, 167–174 doi:10.1016/j.psyneuen.2018.11.014 [CrossRef] PMID:30469083
- Perenboom, R. J. M. & Chorus, A. M. J. (2003). Measuring participation according to the International Classification of Functioning, Disability and Health (ICF). Disability and Rehabilitation, 25, 577–587 doi:10.1080/0963828031000137081 [CrossRef] PMID:12959331
- Polenick, C. A., Leggett, A. N., Webster, N. J., Han, B. H., Zarit, S. H. & Piette, J. D. (2020). Multiple chronic conditions in spousal caregivers of older adults with functional disability: Associations with caregiving difficulties and gains. The Journals of Gerontology. Series B, Psychological Sciences and Social Sciences, 75(1), 160–172 doi:10.1093/geronb/gbx118 [CrossRef] PMID:29029293
- Pranckeviciene, A., Deltuva, V. P., Tamasauskas, A. & Bunevicius, A. (2017). Association between psychological distress, subjective cognitive complaints and objective neuropsychological functioning in brain tumor patients. Clinical Neurology and Neurosurgery, 163, 18–23 doi:10.1016/j.clineuro.2017.10.007 [CrossRef] PMID:29035741
- Roehr, S., Luck, T., Pabst, A., Bickel, H., König, H. H., Lühmann, D., Fuchs, A., Wolfsgruber, S., Wiese, B., Weyerer, S., Mösch, E., Brettschneider, C., Mallon, T., Pentzek, M., Wagner, M., Mamone, S., Werle, J., Scherer, M., Maier, W. & Riedel-Heller, S. G.the AgeCoDe study group. (2017). Subjective cognitive decline is longitudinally associated with lower health-related quality of life. International Psychogeriatrics, 29(12), 1939–1950 doi:10.1017/S1041610217001399 [CrossRef] PMID:28737118
- Roth, D. L., Fredman, L. & Haley, W. E. (2015). Informal caregiving and its impact on health: A reappraisal from population-based studies. The Gerontologist, 55(2), 309–319 doi:10.1093/geront/gnu177 [CrossRef] PMID:26035608
- Ryan, L. H., Smith, J., Antonucci, T. C. & Jackson, J. S. (2012). Cohort differences in the availability of informal caregivers: Are the Boomers at risk?The Gerontologist, 52(2), 177–188 doi:10.1093/geront/gnr142 [CrossRef] PMID:22298747
- Schulz, R. T. & Tompkins, C. A. (2010). Informal caregivers in the United States: Prevalence, caregiver characteristics, and ability to provide care. In National Research Council (Ed.), The role of human factors in home health care: Workshop summary. The National Academies Press.
- Sneed, R. S. & Schulz, R. (2019). Grandparent caregiving, race, and cognitive functioning in a population-based sample of older adults. Journal of Aging and Health, 31, 415–438 doi:10.1177/0898264317733362 [CrossRef] PMID:29254404
- Stacey, A. F., Gill, T. K., Price, K. & Taylor, A. W. (2018). Differences in risk factors and chronic conditions between informal (family) carers and non-carers using a population-based cross-sectional survey in South Australia. BMJ Open, 8(7), e020173 doi:10.1136/bmjopen-2017-020173 [CrossRef] PMID:30037861
- Studart, A. & Nitrini, R. (2016). Subjective cognitive decline: The first clinical mani festation of Alzheimer’s disease?Dementia & Neuropsychologia, 10(3), 170–177 doi:10.1590/S1980-5764-2016DN1003002 [CrossRef] PMID:29213452
- Tales, A., Jessen, F., Butler, C., Wilcock, G., Phillips, J. & Bayer, T. (2015). Subjective cognitive decline. Journal of Alzheimer’s Disease, 48(Suppl. 1), S1–S3 doi:10.3233/JAD-150719 [CrossRef] PMID:26445272
- Tandetnik, C., Hergueta, T., Bonnet, P., Dubois, B. & Bungener, C. (2017). Influence of early maladaptive schemas, depression, and anxiety on the intensity of self-reported cognitive complaint in older adults with subjective cognitive decline. International Psychogeriatrics, 29, 1657–1667 doi:10.1017/S1041610217001119 [CrossRef] PMID:28625189
- Taylor, C. A., Bouldin, E. D. & McGuire, L. C. (2018). Subjective cognitive decline among adults aged ≥45 years – United States, 2015–2016. Morbidity and Mortality Weekly Report, 67, 753–757 doi:10.15585/mmwr.mm6727a1 [CrossRef] PMID:30001562
- Vitaliano, P. P., Zhang, J. & Scanlan, J. M. (2003). Is caregiving hazardous to one’s physical health? A meta-analysis. Psychological Bulletin, 129(6), 946–972 doi:10.1037/0033-2909.129.6.946 [CrossRef] PMID:14599289
- Wang, L. & Tian, T.the Alzheimer’s Disease Neuroimaging Initiative. (2018). Gender differences in elderly with subjective cognitive decline. Frontiers in Aging Neuroscience, 10, 166 doi:10.3389/fnagi.2018.00166 [CrossRef] PMID:29915534
- Wang, X. R., Robinson, K. M. & Carter-Harris, L. (2014). Prevalence of chronic illnesses and characteristics of chronically ill informal caregivers of persons with dementia. Age and Ageing, 43(1), 137–141 doi:10.1093/ageing/aft142 [CrossRef] PMID:24072413
- Wei, Y. C., Huang, L. Y., Chen, C. K., Lin, C., Shyu, Y. C., Chen, Y. L., Huang, W. Y. & Lin, C. P. (2019). Subjective cognitive decline in the community is affected at multiple aspects of mental health and life quality: A cross-sectional study of the community medicine of Keelung Chang Gung Memorial Hospital. Dementia and Geriatric Cognitive Disorders Extra, 9(1), 152–162 doi:10.1159/000497222 [CrossRef] PMID:31011329
- Yap, K. H., Warren, N., Allotey, P. & Reidpath, D. D. (2020). Chronic disease profiles of subjective memory complaints: A latent class analysis of older people in a rural Malaysian community. Aging & Mental Health, 24(5), 709–716 doi:10.1080/13607863.2018.1550632 [CrossRef] PMID:30588848
- Yin, Z., Yan, Z., Liang, Y., Jiang, H., Cai, C., Song, A., Feng, L. & Qiu, C. (2016). Interactive effects of diabetes and impaired kidney function on cognitive performance in old age: A population-based study. BMC Geriatrics, 16, 7 doi:10.1186/s12877-016-0193-6 [CrossRef] PMID:26753625
- Zhang, X., Jiang, X., Han, S., Liu, Q. & Zhou, J. (2019). Type 2 diabetes mellitus is associated with the risk of cognitive impairment: A meta-analysis. Journal of Molecular Neuroscience, 68, 251–260 doi:10.1007/s12031-019-01290-3 [CrossRef] PMID:30949957
- Zlatar, Z. Z., Muniz, M., Galasko, D. & Salmon, D. P. (2018). Subjective cognitive decline correlates with depression symptoms and not with concurrent objective cognition in a clinic-based sample of older adults. The Journals of Gerontology. Series B, Psychological Sciences and Social Sciences, 73, 1198–1202 doi:10.1093/geronb/gbw207 [CrossRef] PMID:28329816
- Zlatar, Z. Z., Muniz, M. C., Espinoza, S. G., Gratianne, R., Gollan, T. H., Galasko, D. & Salmon, D. P. (2018). Subjective cognitive decline, objective cognition, and depression in older Hispanics screened for memory impairment. Journal of Alzheimer’s Disease, 63, 949–956 doi:10.3233/JAD-170865 [CrossRef] PMID:29689718
- Zwar, L., König, H. H. & Hajek, A. (2018). The impact of different types of informal caregiving on cognitive functioning of older caregivers: Evidence from a longitudinal, population-based study in Germany. Social Science & Medicine, 214, 12–19 doi:10.1016/j.socscimed.2018.07.048 [CrossRef] PMID:30134218
Sociodemographic Characteristics of Adults Age ≥45 Years, Behavioral Risk Factor Surveillance System, 2016
| Sex | 0.811 | 0.824 | |||||||
| Men | 46.3 | 40.7 | 48.1 | 46.8 | 46.3 | 12.4 (0.48) | |||
| Women | 53.7 | 59.3 | 51.9 | 53.2 | 53.7 | 12.3 (0.33) | |||
| Age | 0.206 | 0.693 | |||||||
| 45 to 59 | 45.1 | 50.2 | 43.5 | 43.5 | 45.3 | 11.4 (0.59) | |||
| 60 to 69 | 29 | 29.9 | 28.7 | 29 | 29 | 12.8 (0.40) | |||
| 70 to 79 | 17.7 | 14.3 | 18.7 | 17.3 | 17.7 | 12.1 (0.55) | |||
| ≥80 | 8.3 | 5.6 | 9.1 | 10.2 | 8 | 11.2 (0.64) | |||
| Income | 0.274 | ||||||||
| <$15,000 | 9.5 | 8.5 | 9.8 | 22 | 8 | 17.4 (0.69) | |||
| $15,000 to <$50,000 | 40.2 | 39.9 | 40.4 | 48.9 | 39.2 | 12.9 (0.44) | |||
| ≥$50,000 | 50.2 | 51.7 | 49.8 | 29 | 52.7 | 9.6 (0.45) | |||
| Education | |||||||||
| Less than high school | 13.5 | 10.5 | 14.4 | 25.7 | 12 | 16.8 (0.77) | |||
| High school graduate | 30.2 | 30.4 | 30.2 | 30.4 | 30.2 | 12.9 (0.54) | |||
| College or higher | 56.3 | 59.1 | 55.4 | 43.9 | 57.8 | 10.6 (0.33) | |||
| Employment | |||||||||
| Employed | 47.1 | 48.1 | 46.8 | 25.2 | 49.8 | 9.71 (0.43) | |||
| Retired | 32.9 | 29.9 | 33.9 | 32.5 | 33 | 11.3 (0.49) | |||
| Unemployed | 20 | 22 | 19.3 | 42.3 | 17.2 | 16.5 (0.46) | |||
| Race/ethnicity | 0.152 | ||||||||
| White, non-Hispanic | 76.2 | 78.6 | 75.5 | 72.6 | 76.6 | 12.1 (0.31) | |||
| Black, non-Hispanic | 9.3 | 9.8 | 9.2 | 8.4 | 9.4 | 11.3 (0.95) | |||
| Other, non-Hispanic | 6 | 5.4 | 6.2 | 8.1 | 5.7 | 15.2 (1.12) | |||
| Hispanic | 8.5 | 6.2 | 9.2 | 10.8 | 8.2 | 12.8 (1.07) | |||
| Heart disease | 0.981 | ||||||||
| Yes | 11.6 | 11.6 | 11.6 | 21.8 | 10.4 | 11.9 (0.31) | |||
| No | 88.4 | 88.4 | 88.4 | 78.2 | 89.6 | 14.9 (0.65) | |||
| Diabetes | 0.561 | ||||||||
| Yes | 16.7 | 16.2 | 16.8 | 24.8 | 15.7 | 14.3 (0.61) | |||
| No | 83.3 | 83.8 | 83.2 | 75.2 | 84.3 | 11.9 (0.31) | |||
| Obesity | |||||||||
| Yes | 32.9 | 35.2 | 32.1 | 38.6 | 32.2 | 13.5 (0.46) | |||
| No | 67.1 | 64.8 | 67.9 | 61.4 | 67.8 | 11.6 (0.35) | |||
| Current smoking | |||||||||
| Yes | 33.9 | 40 | 319 | 42.7 | 32.4 | 16.5 (0.60) | |||
| No | 66.1 | 60 | 68.1 | 57.3 | 67.6 | 11.8 (0.45) | |||
| Physical activity | 0.058 | ||||||||
| Yes | 69.2 | 71.3 | 68.5 | 52.2 | 71.3 | 10.2 (0.32) | |||
| No | 30.8 | 28.7 | 31.5 | 47.8 | 28.7 | 15.9 (0.51) | |||
| Alcohol use (mean, |
2.00 (0.04) | 1.95 (0.07) | 2.01 (0.04) | 0.100 | 2.16 (0.11) | 1.98 (0.04) | 0.400 | 0.106 |
|
Caregiving Characteristics Overall and Among Men and Women
| Caregiver relationship | ||||
| Parent | 37.1 | 27.3 | 33.6 | |
| Child | 1.4 | 26.2 | 24.2 | |
| Spouse/partner | 22.7 | 22.4 | 16.7 | |
| Other relative | 29.8 | 24.1 | 25.6 | |
| Hours spent per week | ||||
| ≤8 | 54.1 | 58.6 | 50.9 | |
| 9 to 19 | 13.1 | 12.8 | 13.4 | |
| 20 to 39 | 11.2 | 10.2 | 12 | |
| ≥40 | 21.6 | 18.5 | 23.7 | |
Overall Association Between Caregiving, Mental Distress, and Subjective Cognitive Decline (SCD) Among the Overall Sample, Men, and Women Aged ≥45 Years, Behavioral Risk Factor Surveillance System, 2016
| Caregiving and poor mental health (β) | ||||
| Mental distress and SCD | ||||
| Caregiving and SCD | 1.36 [0.92, 1.78] | 0.127 | ||
| Caregiving and poor mental health (β) | ||||
| Mental distress and SCD | ||||
| Caregiving and SCD | 1.56 [0.93, 2.63] | 0.094 | ||
| Caregiving and poor mental health (β) | 0.60 [–0.78, 1.98] | 0.396 | ||
| Mental distress and SCD | ||||
| Caregiving and SCD | 1.15 [0.91, 1.45] | 0.246 | 1.34 [0.74, 2.42] | 0.336 |