Summary
Background
Hydroxychloroquine, a drug commonly used in the treatment of rheumatoid arthritis, has received much negative publicity for adverse events associated with its authorisation for emergency use to treat patients with COVID-19 pneumonia. We studied the safety of hydroxychloroquine, alone and in combination with azithromycin, to determine the risk associated with its use in routine care in patients with rheumatoid arthritis.
Methods
In this multinational, retrospective study, new user cohort studies in patients with rheumatoid arthritis aged 18 years or older and initiating hydroxychloroquine were compared with those initiating sulfasalazine and followed up over 30 days, with 16 severe adverse events studied. Self-controlled case series were done to further establish safety in wider populations, and included all users of hydroxychloroquine regardless of rheumatoid arthritis status or indication. Separately, severe adverse events associated with hydroxychloroquine plus azithromycin (compared with hydroxychloroquine plus amoxicillin) were studied. Data comprised 14 sources of claims data or electronic medical records from Germany, Japan, the Netherlands, Spain, the UK, and the USA. Propensity score stratification and calibration using negative control outcomes were used to address confounding. Cox models were fitted to estimate calibrated hazard ratios (HRs) according to drug use. Estimates were pooled where the I2 value was less than 0·4.
Findings
The study included 956 374 users of hydroxychloroquine, 310 350 users of sulfasalazine, 323 122 users of hydroxychloroquine plus azithromycin, and 351 956 users of hydroxychloroquine plus amoxicillin. No excess risk of severe adverse events was identified when 30-day hydroxychloroquine and sulfasalazine use were compared. Self-controlled case series confirmed these findings. However, long-term use of hydroxychloroquine appeared to be associated with increased cardiovascular mortality (calibrated HR 1·65 [95% CI 1·12–2·44]). Addition of azithromycin appeared to be associated with an increased risk of 30-day cardiovascular mortality (calibrated HR 2·19 [95% CI 1·22–3·95]), chest pain or angina (1·15 [1·05–1·26]), and heart failure (1·22 [1·02–1·45]).
Interpretation
Hydroxychloroquine treatment appears to have no increased risk in the short term among patients with rheumatoid arthritis, but in the long term it appears to be associated with excess cardiovascular mortality. The addition of azithromycin increases the risk of heart failure and cardiovascular mortality even in the short term. We call for careful consideration of the benefit–risk trade-off when counselling those on hydroxychloroquine treatment.
Funding
National Institute for Health Research (NIHR) Oxford Biomedical Research Centre, NIHR Senior Research Fellowship programme, US National Institutes of Health, US Department of Veterans Affairs, Janssen Research and Development, IQVIA, Korea Health Industry Development Institute through the Ministry of Health and Welfare Republic of Korea, Versus Arthritis, UK Medical Research Council Doctoral Training Partnership, Foundation Alfonso Martin Escudero, Innovation Fund Denmark, Novo Nordisk Foundation, Singapore Ministry of Health’s National Medical Research Council Open Fund Large Collaborative Grant, VINCI, Innovative Medicines Initiative 2 Joint Undertaking, EU’s Horizon 2020 research and innovation programme, and European Federation of Pharmaceutical Industries and Associations.
Evidence before this study
Added value of this study
This study uses state-of-the-art methods to control for residual confounding and bias and shows comparable results across 14 international health databases. Hydroxychloroquine does not seem to confer increased risk when used in patients with rheumatoid arthritis without contraindications in the short term (up to 30 days) compared with sulfasalazine, but confers an increased risk of cardiovascular mortality when used long term. Short-term treatment with hydroxychloroquine plus azithromycin appears to be associated with elevated risk of cardiovascular mortality, angina, and heart failure compared with hydroxychloroquine plus amoxicillin.
Implications of all the available evidence
Short-term use of hydroxychloroquine appears to confer no increased risk in patients with rheumatoid arthritis without contraindications, but hydroxychloroquine in combination with azithromycin appears to be associated with serious cardiovascular adverse events and should therefore be used with caution.
Introduction
,
,
,
,
Unfortunately, the exponential generation of research into hydroxychloroquine has led to confusion in the rheumatological community regarding the safety implications of hydroxychloroquine within its traditional uses.
showing faster recovery and reduction in viral load in patients treated with high-dose hydroxychloroquine plus azithromycin, a macrolide antibiotic, compared with patients receiving standard treatment available at the time. This report led to widespread use of high-dose hydroxychloroquine either alone or with azithromycin. Subsequently, serious cardiac adverse events associated with QT segment prolongation that could lead to potentially lethal arrhythmia and cardiovascular-related death were identified in patients taking hydroxychloroquine in several health-care centres in the USA and Brazil.
,
,
,
Because of these reports of increased risk, emergency authorisation of hydroxychloroquine by medicines regulators was retracted, statements cautioning against hydroxychloroquine use were released, and randomised trials were stopped.
,
,
,
,
,
,
Before the COVID-19 pandemic, evidence for hydroxychloroquine safety was largely found in retrospective case series and case reports, or within pharmaceutical adverse events registers.
,
,
Azithromycin and macrolides in general are also known to induce cardiotoxicity and to interact with other drugs that prolong QTc.
,
,
The combination of minimal large-scale hydroxychloroquine safety studies before this pandemic, and the extensive research suggesting risks associated with hydroxychloroquine use that has been produced during 2020 is of great concern to both patients and clinicians. We therefore aimed to assess the safety of hydroxychloroquine alone compared with sulfasalazine and of hydroxychloroquine in combination with azithromycin (compared with hydroxychloroquine in combination with amoxicillin), in part to provide clarity for patients taking hydroxychloroquine for rheumatoid arthritis.
Methods
Study design and participants
for observational drug safety research to estimate the safety of hydroxychloroquine alone or in combination with macrolide antibiotics in patients with rheumatoid arthritis. Sulfasalazine and amoxicillin were chosen as active comparators because they have similar indications as the target treatments (hydroxychloroquine and azithromycin, respectively). Participants were included if they had a history of rheumatoid arthritis (a condition occurrence or observation indicating rheumatoid arthritis any time before or on the same day as therapy initiation), were aged 18 years or older at the index event, and had at least 365 days of continuous observation time before the index event.
As a secondary analysis, a self-controlled case series was used to estimate the safety of hydroxychloroquine in the wider population, including patients without rheumatoid arthritis. For this analysis, all prevalent users of hydroxychloroquine were included, regardless of rheumatoid arthritis status or indication.
All data partners received approval or waiver from their institutional review boards in accordance with their institutional governance guidelines. The full study protocol is available online.
Data sources
Electronic health records (EHRs) and administrative claims data were mapped to the Observational Medical Outcomes Partnership common data model (version 5.0 or higher) and analysed in a distributed network as part of an international effort with the Observational Health Data Science and Informatics community, including 14 databases: IQVIA (Durham, NC, USA) Disease Analyzer Germany (ambulatory electronic medical record [EMR] from Germany); Japanese Medical Data Center Claims Database (Tokyo, Japan); Integrated Primary Care Information (IPCI; Rotterdam, Netherlands; primary care EMR); Information System for the Development of Research in Primary Care (SIDIAP; Barcelona, Spain; primary care EMR); Clinical Practice Research Datalink (CPRD; London, UK) and IQVIA UK (London, UK) Integrated Medical Record Data (IMRD; primary care EMRs); and IBM MarketScan (Somers, NY, USA) Commercial Claims and Encounters (CCAE), Optum (Eden Prairie, MN, USA) de-identified Clinformatics Data Mart Database (Clinformatics), Optum EHR (Optum de-identified Electronic Health Record dataset), IBM MarketScan Medicare Supplemental Database (MDCR), IBM MarketScan Multi-State Medicaid Database (MDCD), IQVIA Open Claims, US Department of Veterans Affairs (VA; Salt Lake City, UT, USA), and IQVIA US Ambulatory EMR (USA).
Study period and outcomes
For a longer-term, on-treatment analysis, follow-up started 1 day after the index date and continued until the earliest of: outcome of interest, loss to follow-up, or discontinuation, with an added washout time of 14 days. Continued use of the same treatment was inferred by allowing up to 90-day gaps between dispensing or prescription records. Additional detail on the exposure cohorts is available in the appendix (pp 5–8).
For self-controlled case series, periods of persistent exposure to hydroxychloroquine were generated allowing up to 90-day gaps between dispensing or prescription records. Patients were followed up for their entire observation time (eg, from enrolment to disenrolment in each database), and rates of each of the outcomes calculated in periods of exposure and non-exposure time.
and are detailed in the appendix (pp 8–9). Face validity for each of the outcome cohorts was further reviewed and compared with previous clinical knowledge and existing literature.
A full list of the codes that were used to identify negative control outcomes and details on covariate and confounder identification are provided in the appendix (pp 10–11).
Statistical analysis
Baseline patient characteristics were constructed for inclusion as potentially confounding covariates.
Predictor variables included were based on all observed patient characteristics as available in each data source, including conditions, procedures, visits, observations, and measurements. We plotted the propensity score distribution and assessed covariate balance expressed as the standardised difference of the mean for every covariate before and after propensity score stratification. A standardised difference of more than 0·1 indicated a non-negligible imbalance between exposure cohorts.
Cox proportional hazards models conditioned on the propensity score strata were fitted to estimate hazard ratios (HRs) according to treatment status. Negative control outcomes analyses and empirical calibration were used to minimise potential unresolved confounding, with calibrated HRs and 95% CIs estimated.
,
The standard errors of the database-specific estimates were adjusted to incorporate estimate variation across databases, where the across-database variance was estimated by comparing each database-specific result to that of an inverse-variance, fixed-effects meta-analysis. No meta-analysis was done where I2 for a given drug–outcome pair was 0·4 or more. Of note, when running analysis in a distributed network, it was not possible to link across datasets, and to know the extent of overlap between data.
All self-controlled case series were run using the self-controlled case series package.
The full source code for analyses is available online.
EU PAS registration: hydroxychloroquine safety and potential efficacy as an antiviral prophylaxis in light of potential wide-spread use in COVID-19: a multinational, large-scale network cohort and self-controlled case series study.
Role of the funding source
The funders of the study had no role in study design, data collection, data analysis, data interpretation, writing of the manuscript, or the decision to submit for publication. All authors had full access to aggregated data in the study, and the lead and senior authors (JCEL, JW, PRy, and DP-A) had final responsibility for the decision to submit for publication.
Results
Table 1Baseline characteristics of users of HCQ versus SSZ, and HCQ plus AZM versus HCQ plus AMX after propensity score stratification in the CCAE database
Percentages might not sum to 100% because of rounding. An example of one dataset is included. AMX=amoxicillin. AZM=azithromycin. CCAE=IBM Commercial Claims and Encounters. HCQ=hydroxychloroquine. SSZ=sulfasalazine.
Table 2Patient counts, event counts, and incidence rates of key outcomes according to HCQ versus SSZ use
AmbEMR=IQVIA Ambulatory EMR. CCAE=IBM Commercial Claims and Encounters. CPRD=Clinical Practice Research Datalink. DAGermany=IQVIA Disease Analyzer Germany. EMR=electronic medical record. HCQ=hydroxychloroquine. IMRD=IQVIA UK Integrated Medical Record Data. MDCD=IBM Multi-state Medicaid. MDCR=IBM Medicare Supplemental Database. NA=non-applicable (not reported because of failed diagnostics or on-treatment follow-up unavailable). OptumEHR=Optum de-identified Electronic Health Record. SSZ=sulfasalazine. VA=US Department of Veterans Affairs.
Table 3Patient counts, event counts, and incidence rates of key outcomes according to HCQ plus AZM versus HCQ plus AMX use
AmbEMR=IQVIA Ambulatory EMR. AMX=amoxicillin. AZM=azithromycin. CCAE=IBM Commercial Claims and Encounters. CPRD=Clinical Practice Research Datalink. DAGermany=IQVIA Disease Analyzer Germany. EMR=electronic medical record. HCQ=hydroxychloroquine. IMRD=IQVIA UK Integrated Medical Record Data. MDCD=IBM Multi-state Medicaid. MDCR=IBM Medicare Supplemental Database. NA=non-applicable (not reported because of failed diagnostics or on-treatment follow-up unavailable). OptumEHR=Optum de-identified Electronic Health Record. VA=US Department of Veterans Affairs.
EU PAS registration: hydroxychloroquine safety and potential efficacy as an antiviral prophylaxis in light of potential wide-spread use in COVID-19: a multinational, large-scale network cohort and self-controlled case series study.
For all-cause mortality in the on-treatment analysis, the I2 value was 0·71, indicating substantial heterogeneity between results and therefore a summary estimate was not reported. The same is true for gastrointestinal bleeding (I2=0·57) and stroke (I2=0·58) in the on-treatment analysis.

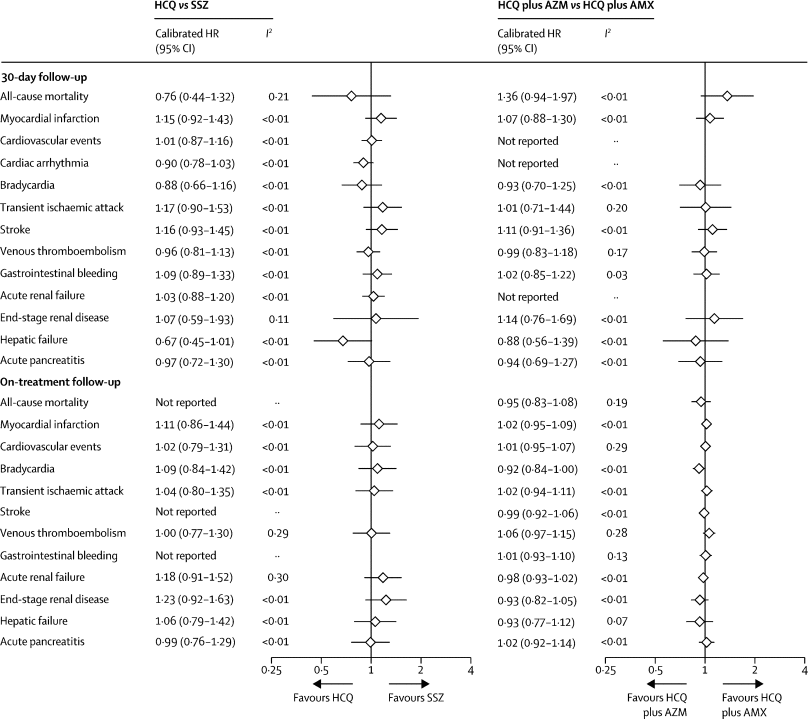
Figure 1Meta-analytic estimates for HCQ versus SSZ and HCQ plus AZM versus HCQ plus AMX new users during 30-day (intention-to-treat) and long-term (on-treatment) follow-up
AMX=amoxicillin. AZM=azithromycin. HCQ=hydroxychloroquine. HR=hazard ratio. SSZ=sulfasalazine.

Figure 2Source-specific and meta-analytic-specific severe adverse event risk estimates for HCQ versus SSZ and HCQ plus AZM versus HCQ plus AMX new users during 30-day (intention-to-treat) follow-up
AmbEMR=IQVIA Ambulatory EMR. AMX=amoxicillin. AZM=azithromycin. CCAE=IBM Commercial Claims and Encounters. CPRD=Clinical Practice Research Datalink. DAGermany=IQVIA Disease Analyzer Germany. EMR=electronic medical record. HCQ=hydroxychloroquine. HR=hazard ratio. IMRD=IQVIA UK Integrated Medical Record Data. MDCD=IBM Multi-state Medicaid. MDCR=IBM Medicare Supplemental Database. OptumEHR=Optum de-identified Electronic Health Record. SSZ=sulfasalazine. VA=US Department of Veterans Affairs.

Figure 3Source-specific and meta-analytic specific severe adverse event risk estimates for HCQ versus SSZ and HCQ plus AZM versus HCQ plus AMX new users during long-term (on-treatment) follow-up
AmbEMR=IQVIA Ambulatory EMR. AMX=amoxicillin. AZM=azithromycin. CCAE=IBM Commercial Claims and Encounters. CPRD=Clinical Practice Research Datalink. DAGermany=IQVIA Disease Analyzer Germany. EMR=electronic medical record. HCQ=hydroxychloroquine. HR=hazard ratio. IMRD=IQVIA UK Integrated Medical Record Data. MDCD=IBM Multi-state Medicaid. MDCR=IBM Medicare Supplemental Database. OptumEHR=Optum de-identified Electronic Health Record. SSZ=sulfasalazine. VA=US Department of Veterans Affairs.
Table 4Summary of self-controlled case series results for HCQ
CCAE=IBM Commercial Claims and Encounters. CPRD=Clinical Practice Research Datalink. HCQ=hydroxychloroquine. JMDC=Japanese Medical Data Center. MDCD=IBM Multi-state Medicaid. MDCR=IBM Medicare Supplemental Database. NA=non-applicable (not reported because of failed diagnostics or on-treatment follow-up unavailable). VA=US Department of Veterans Affairs.
Discussion
To our knowledge, this study is the largest ever analysis of the safety of hydroxychloroquine and hydroxychloroquine plus azithromycin worldwide, examining more than 950 000 hydroxychloroquine and more than 300 000 hydroxychloroquine plus azithromycin users, respectively. Short-term (up to 30 days) hydroxychloroquine treatment among patients with rheumatoid arthritis showed no excess risk of any of the considered severe adverse events compared with sulfasalazine. Short-term treatment is also proposed for COVID-19 therapy and might be informed by the experience of treatment in patients with rheumatoid arthritis. By comparison, long-term hydroxychloroquine therapy appears to be associated with a relative risk increase in cardiovascular-related mortality compared with a roughly equivalent rheumatoid arthritis therapy (sulfasalazine; calibrated HR 1·65 [95% CI 1·12–2·44]). Perhaps more worryingly, compared with hydroxychloroquine plus amoxicillin, significant risks were identified for the combination of hydroxychloroquine plus azithromycin even in the short term: increased risk of angina or chest pain (calibrated HR 1·15 [95% CI 1·05–1·26]) and heart failure (1·22 [1·02–1·45]), and a doubled risk of cardiovascular mortality in the first month of treatment (2·19 [1·22–3·94]).
,
Furthermore, interrogation of the US Food and Drug Administration Adverse Event Reporting System database identified 357 adverse events reported for chloroquine.
20% of the events reported were cardiac and included arrhythmia, sudden cardiac death, or heart failure.
,
In this study, a relative risk of 2·19 (95% CI 1·22–3·94) for cardiovascular death was seen even with short-term hydroxychloroquine plus azithromycin combination therapy, probably arising through their synergistic effects on QT length and subsequent induction of lethal arrhythmia. Considering that hydroxychloroquine and azithromycin are both contraindicated for use in patients with cardiac arrhythmias, this study assumes that clinicians are prescribing these medications for patients as per existing labelling advice. It is therefore concerning that cardiovascular effects were still seen in our study populations, possibly indicating that the true risks of these drugs are understated in the analysis.
It is important to identify potential sources of bias that could limit the study. The analyses are predicated on observing the presence of exposure, outcomes, and covariates in the data, or inferring their absence based on an assumption of complete data capture during a defined observation period during which a person is not expected to be lost to follow-up. In this regard, although there were no missing data that required imputation, each binary variable is subject to potential misclassification error, and the sensitivity and specificity of these variables in each database are unknown. Because of the nature of sudden cardiac death, capturing the true cause of cardiovascular-related mortality is difficult. Although we examined various aspects of cardiac complications as captured by diagnosis codes, the accuracy of evaluations of QT prolongation, ventricular tachycardia, or other arrhythmias would probably be improved with precise electrocardiogram measurements. Exposure misclassification can occur as a result of non-adherence or non-compliance with either treatment and thus could bias the results in either direction, and outcome misclassification might exist because of incomplete or incorrect recording of severe adverse events. Baseline covariates might also be subject to measurement error and, although observing balance on all baseline characteristics after propensity score adjustment provides reassurance that the risk of confounding has been reduced, there remains potential for confounding in any given source for differential misclassification. The consistency of findings across heterogeneous patient populations with disparate data capture processes mitigates this concern. Within the study design, use of routine health-care data in populations across four continents, and including all adults with rheumatoid arthritis was used to minimise selection bias. The self-controlled case series analysis was also added to investigate all users of hydroxychloroquine as an external validation of the hydroxychloroquine findings in the rheumatoid arthritis population via the new user design. To investigate systematic error, study diagnostics were evaluated before unblinding results through interrogation of negative controls.
,
,
,
We ensured that, when investigating covariate balance after propensity score stratification and matching and before unblinding study results, we did not see unbalanced proportions of patients with a diagnosis of SLE between the groups. Negative control outcome analyses to assess for systematic error also did not identify any residual unobserved confounding in the propensity score analysis, adjusting for thousands of variables within the large-scale propensity score model. Although we have balanced for the coexistence of other conditions and medications through propensity scores, and we tested for residual unobserved confounding to ensure groups were balanced, no direct measure of severity of rheumatoid arthritis was drawn for patients at baseline. The cohort was made from patients who were new users of both hydroxychloroquine and sulfasalazine with a diagnosis of rheumatoid arthritis and without medication use in the previous 365 days, but the potential for differences in baseline rheumatoid arthritis severity not recorded in routinely collected data is also a limitation of the study.
Another criticism is the choice of sulfasalazine as an active comparator. Both hydroxychloroquine and sulfasalazine are second-line conventional synthetic disease-modifying antirheumatic drugs in the treatment of patients with rheumatoid arthritis, used in addition to, or instead of methotrexate. Although they are not fully equivalent to each other, and no drug can be an exact match, they are each the closest comparator treatment to the other. Appreciating they are not truly equivalent, we took care to ensure that propensity score stratification and negative control analysis for any systematic error ensured that the two groups were as balanced as possible to minimise confounding.
Another potential limitation in this study is the potential for patients to be included in more than one dataset in the USA. Although we ran meta-analyses, which assume populations are independent, we highlight that we are likely to have underestimated variance in our meta-analytic estimates. We also acknowledge the limitation that although 14 databases were used in total, mortality analysis was restricted to databases with good coverage of this outcome (ie CPRD, IMRD, IPCI, VA, and Clinformatics). Similarly, as we do not know the baseline risk of serious adverse events within this population, we cannot report absolute risk of these events in patients with rheumatoid arthritis, and this limitation must be acknowledged.
Contributors
OA, HA, PB, AVM, MTFA, TMA, PC, ACC, AD, DD, KF, LH, SKe, SKh, SKo, RM, PM, DRM, DN, FN, AO, AP-U, JX, SMKS, DV, HW, LZ, and JCEL searched the literature. JCEL, JW, GH, KK, TD-S, EB, JvdL, CR, JR, PRi, MSc, AGS, AS, MSp, MAS, MdW, SCY, PRy, and DP-A were involved in the study design and concept. JCEL, JW, MAS, GH, AVM, DV, FN, PRi, PRy, and DP-A were responsible for data interpretation, with assistance from JW, AO, JH, LH, GH, SKe, SKh, FN, RWP, AP-U, CR, PRi, AGS, and MAS. JCEL, JW, MMC, AD, SLDV, SF-B, CGL, KEL, RM, MEM, HM-S, MM, GAR, CR, JR, PRi, MSc, SS, AGS, AS, MSp, MAS, COT, DV, MdW, SCY, OZ, PRy, and DP-A analysed the data. JCEL, JW, PRy, and DP-A wrote the manuscript. The corresponding author confirms that all authors read and approved the final manuscript.
Declaration of interests
JW is an employee and shareholder at Janssen Research and Development. SLDV reports grants from Anolinx, Astellas Pharma, AstraZeneca Pharmaceuticals, Boehringer Ingelheim International, Celgene, Eli Lilly, Genentech, Genomic Health, Gilead Sciences, GlaxoSmithKline, Innocrin Pharmaceuticals, Janssen Pharmaceuticals, Kantar Health, Myriad Genetic Laboratories, Novartis International, Parexel International through the Western Institute for Biomedical Research, the non-profit corporation associated with the Department of Veterans Affairs (Salt Lake City, UT, USA; outside the submitted work). GH reports grants from the US National Library of Medicine and Janssen Research (outside the submitted work). BSK-H reports grants from the Innovation Fund Denmark (5153-00002B) and Novo Nordisk Foundation (NNF14CC0001; outside the submitted work). SKh is an employee of and stockholder in AstraZeneca. JvdL reports grants from the Innovative Medicines Initiative (during the conduct of the study). AVM is an employee of RTI Health Solutions, a unit of the independent, non-profit research organisation RTI international. DRM reports funding support from the Wellcome Trust, the UK National Institute for Health Research (NIHR), Scottish Chief Scientist Office, and Tenovus Scotland (outside the submitted work). MM and MdW report grants from the Innovative Medicines Initiative (during the conduct of the study). FN was an employee of AstraZeneca until September, 2019. GAR is an employee of Janssen Research and Development. PRi reports grants from the Innovative Medicines Initiative and Janssen Research and Development (during the conduct of the study). MSc is an employee of and shareholder in Janssen Research and Development. JH, JR, RM, PRy, MSc, and AGS are employees of Janssen Research and Development and shareholders in Johnson & Johnson. AS, LH, and MMC are employees of Janssen Research and Development. HM-S, KK, CR, COT, and SS are employees of IQVIA. MAS reports grants from the US National Science Foundation and US National Institutes of Health, and personal fees from Janssen Research and Development (during the conduct of the study). DV reports personal fees from Bayer (outside the submitted work) and is a full-time employee of Bayer. SCY reports grants from the Korean Ministry of Health and Welfare and the Korean Ministry of Trade, Industry and Energy (during the conduct of the study). DP-A reports grants from Amgen, UCB Biopharma, and Les Laboratoires Servier; personal fees (paid to his department) from Amgen and UCB Biopharma; and support for training programmes organised by his department from Innovative Medicines Initiative-funded European Health Data and Evidence Network and European Medical Information Framework consortiums, and Synapse Management Partners. All other authors declare no competing interests.
Data sharing
Acknowledgments
Supplementary Material
References
- 1.
Chloroquine and hydroxychloroquine as available weapons to fight COVID-19.
Int J Antimicrob Agents. 2020; 55105932
- 2.
Effects of chloroquine on viral infections: an old drug against today’s diseases?.
Lancet Infect Dis. 2003; 3: 722-727
- 3.
Virus glycosylation: role in virulence and immune interactions.
Trends Microbiol. 2007; 15: 211-218
- 4.
New insights on the antiviral effects of chloroquine against coronavirus: what to expect for COVID-19?.
Int J Antimicrob Agents. 2020; 55105938
- 5.
Remdesivir and chloroquine effectively inhibit the recently emerged novel coronavirus (2019-nCoV) in vitro.
Cell Res. 2020; 30: 269-271
- 6.
Hydroxychloroquine and azithromycin as a treatment of COVID-19: results of an open-label non-randomized clinical trial.
Int J Antimicrob Agents. 2020; 56105949
- 7.
Risk of QT interval prolongation associated with use of hydroxychloroquine with or without concomitant azithromycin among hospitalized patients testing positive for coronavirus disease 2019 (COVID-19).
JAMA Cardiol. 2020; ()
- 8.
Considerations for drug interactions on QTC in exploratory COVID-19 (coronavirus disease 2019) treatment.
Circulation. 2020; 141: e906-e907
- 9.
The QT interval in patients with COVID-19 treated with hydroxychloroquine and azithromycin.
Nat Med. 2020; 26: 808-809
- 10.
Effect of high vs low doses of chloroquine diphosphate as adjunctive therapy for patients hospitalized with severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection: a randomized clinical trial.
JAMA Netw Open. 2020; 3e208857
- 11.
Statement from the Chief Investigators of the Randomised Evaluation of COVid-19 thERapY (RECOVERY) Trial on hydroxychloroquine, 5 June 2020.
- 12.
“Solidarity” clinical trial for COVID-19 treatments update on hydroxychloroquine.
- 13.
Double blind controlled phase III multicenter clinical trial with interferon gamma in rheumatoid arthritis.
Rheumatol Int. 1992; 12: 175-185
- 14.
COVID-19: reminder of the risks of chloroquine and hydroxychloroquine.
- 15.
FDA revokes Emergency Use Authorization for chloroquine phosphate and hydroxychloroquine sulfate.
- 16.
Safety of synthetic and biological DMARDs: a systematic literature review informing the 2019 update of the EULAR recommendations for the management of rheumatoid arthritis.
Ann Rheum Dis. 2020; 79: 760-770
- 17.
Impact of adverse events associated with medications in the treatment and prevention of rheumatoid arthritis.
Clin Ther. 2019; 41: 1376-1396
- 18.
Data mining and safety analysis of drugs for novel coronavirus pneumonia treatment based on FAERS: chloroquine phosphate.
Herald Med. 2020; 39: 505-512
- 19.
Cardiac complications attributed to chloroquine and hydroxychloroquine: a systematic review of the literature.
Drug Saf. 2018; 41: 919-931
- 20.
Antimalarial-induced cardiomyopathy: a systematic review of the literature.
Lupus. 2018; 27: 591-599
- 21.
The cardiotoxicity of macrolides: a systematic review.
Pharmazie. 2010; 65: 631-640
- 22.
Azithromycin and the risk of cardiovascular death.
N Engl J Med. 2012; 366: 1881-1890
- 23.
Cardiac risks associated with antibiotics: azithromycin and levofloxacin.
Expert Opin Drug Saf. 2015; 14: 295-303
- 24.
ENCePP guide on methodological standards in pharmacoepidemiology, revision 8.
- 25.
The book of OHDSI.
Observational Health Data Sciences and Informatics,
2020 - 26.
Comprehensive comparative effectiveness and safety of first-line antihypertensive drug classes: a systematic, multinational, large-scale analysis.
Lancet. 2019; 394: 1816-1826
- 27.
Accuracy of an automated knowledge base for identifying drug adverse reactions.
J Biomed Inform. 2017; 66: 72-81
- 28.
New insights into mechanisms of therapeutic effects of antimalarial agents in SLE.
Nat Rev Rheumatol. 2012; 8: 522-533
- 29.
Evaluating large-scale propensity score performance through real-world and synthetic data experiments.
Int J Epidemiol. 2018; 47: 2005-2014
- 30.
Balance diagnostics for comparing the distribution of baseline covariates between treatment groups in propensity-score matched samples.
Stat Med. 2009; 28: 3083-3107
- 31.
Robust empirical calibration of p-values using observational data.
Stat Med. 2016; 35: 3883-3888
- 32.
Interpreting observational studies: why empirical calibration is needed to correct p-values.
Stat Med. 2014; 33: 209-218
- 33.
Massive parallelization of serial inference algorithms for a complex generalized linear model.
ACM Trans Model Comput Simul. 2013; 23: 1-17
- 34.
Meta-analysis in clinical trials.
Control Clin Trials. 1986; 7: 177-188
- 35.
Multiple self-controlled case series for large-scale longitudinal observational databases.
Biometrics. 2013; 69: 893-902
- 36.
EU PAS registration: hydroxychloroquine safety and potential efficacy as an antiviral prophylaxis in light of potential wide-spread use in COVID-19: a multinational, large-scale network cohort and self-controlled case series study.
- 37.
Antimalarial treatment may have a time-dependent effect on lupus survival: data from a multinational Latin American inception cohort.
Arthritis Rheum. 2010; 62: 855-862
- 38.
Hydroxychloroquine reduces risk of incident diabetes mellitus in lupus patients in a dose-dependent manner: a population-based cohort study.
Rheumatology. 2015; 54: 1244-1249
- 39.
Hydroxychloroquine and risk of diabetes in patients with rheumatoid arthritis.
JAMA. 2007; 298: 187-193
Article Info
Publication History
Published: August 21, 2020
Identification
Copyright
© 2020 The Author(s). Published by Elsevier Ltd.